By Dr. Guy-André Pelouze, a French cardiovascular and thoracic surgeon
The new dietary recommendations from the U.S. administration represent a discreet and cautious break with the past emphasis on “low-fat” diets, the campaign against saturated fats, and the vegan bias promoted in the name of saving the planet, among other trends. In reality, the Trump administration has just revealed the elephant in the kitchen: ultra-processed food (UPF), which reigns supreme in our factories, supermarkets, and kitchens.
One might have expected this shift to generate strong scientific and public interest. However, this has not been the case, and three reactions are particularly surprising.
Three Surprising Reactions to the New Focus
First, there is the political polarization surrounding the discussion of this topic within the United States itself. Many commentators approach questions of calories, sugar, meat, and other food-related issues through an ideological lens. Most importantly, they fail to see the elephant in the room.
Second, there has been an extraordinary silence across Europe. Instead of welcoming a renewed focus on minimally processed foods—long recognized as a factor contributing to longevity in many Mediterranean regions and potentially an advantage for European agricultural products—European countries appear reluctant to reconsider their own dietary recommendations. More precisely, the most recent editions of these guidelines are marked by highly uncertain claims because they rely heavily on observational studies. Furthermore, risk assessments associated with specific foods are largely blind to the role of ultra-processed products. Systems such as Nutri-Score have serious limitations in this regard. The elephant in the European kitchen therefore remains concealed. Applying the NOVA classification of foods (1) could help reassess the progression of UPF consumption.
Third, there has been a striking academic silence worldwide. Editorials and opinion pieces tend instead to lament recent cuts to research funding. One only needs to read Nature to see this trend. This diversion toward institutional constraints contributes to an informational fog that does little to serve public health. Simply stating that we do not fully understand why ultra-processed foods are so strongly associated with excess mortality and, consequently, obesity (2) is not sufficient to delay alternative public-health action.
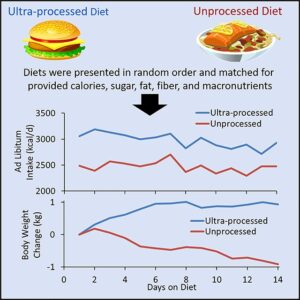
The Urgent Need for Evidence-Based Reform
Yet there is much to be done in the field of dietary advice—that is, the diets recommended to populations in developed countries—based on robust and carefully controlled evidence. The quality of the information underlying current recommendations remains poor. We must abandon the polite assumption that large observational databases from Harvard or elsewhere can produce evidence free from confounding bias or from the multiple analytical manipulations often required to obtain the desired results.
There is also no compelling reason why processed foods should not be subject to a higher level of safety assessment than the FDA’s simple GRAS (“Generally Recognized as Safe”) designation. After all, the foods that have been recognized as safe through long-term human adaptation are plants, animals, and fish in their fresh or minimally prepared culinary forms—not highly processed industrial products.
Acknowledging Hard Truths and Moving Beyond Orthodoxy
In reality, these guidelines—by exposing the nature of ultra-processed foods as a mixture of sugar, polyunsaturated fats, numerous additives, fillers, and other components assembled into products lacking a natural biological matrix—have stirred a hornet’s nest. Ultra-processed foods are widely discussed, yet few are truly willing to reduce their role in modern diets. The economic and political stakes are simply too high.
We will have to acknowledge that some ideas previously presented as nutritional truths may be far from beneficial to public health. For example, P. W. Siri-Tarino (3) provided strong evidence that saturated fat intake is not associated with a higher relative risk of coronary heart disease or stroke. It should be recognized that saturated fats appear largely neutral from a cardiovascular risk perspective in individuals at low cardiovascular risk (4), while in higher-risk populations the absolute benefit of reducing saturated fat intake remains modest. This does not mean that replacing saturated fats with mono- or polyunsaturated fats would be unjustified in patients with symptomatic atherosclerosis, for example (5).
From a metabolic standpoint, impaired carbohydrate metabolism appears to be a major driver of central obesity, chronic inflammation, and therefore cardiovascular disease and cancer. A systematic review estimates the global prevalence of insulin resistance at 26.53%, with values ranging from approximately 26% to 30% across populations and geographic regions (6).
We can also consider the question of cancer, which has recently been reassessed (7). Cancers are undoubtedly driven by age, genetics, and exposure to carcinogens. In developed countries, tobacco smoking, alcohol consumption, and obesity remain the most prevalent carcinogenic factors. By contrast, red meat consumption (below 300 g per week) does not appear among the top ten risk factors. This distinction is essential for designing effective health policies.
All of this may be difficult to accept. Ultimately, the discussion should focus on foods rather than isolated nutrients—a point clearly emphasized by Arne Astrup in a 2020 article (8).
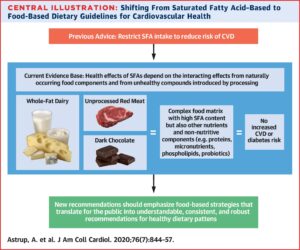
Will these changes occur, or will there be yet another attempt to silence ideas that challenge the prevailing orthodoxy, along with the continued reliance on observational studies that consume so many research resources? Only time will tell. Public health, however, cannot afford another decade of nutritional inertia.
1 https://pmc.ncbi.nlm.nih.gov/articles/PMC10261019/
2 https://pubmed.ncbi.nlm.nih.gov/31105044/
3 https://www.sciencedirect.com/science/article/pii/S0002916523016726?via%3Dihub
4 https://www.acpjournals.org/doi/10.7326/ANNALS-25-02229
6 https://pmc.ncbi.nlm.nih.gov/articles/PMC12411212/
7 https://www.thelancet.com/journals/lancet/article/piis0140-6736(22)01438-6/fulltext
8 https://www.jacc.org/doi/10.1016/j.jacc.2020.05.077
Disclaimer: www.BrusselsReport.eu will under no circumstance be held legally responsible or liable for the content of any article appearing on the website, as only the author of an article is legally responsible for that, also in accordance with the terms of use.













